 How Does Health Vary Across the Lifespan in the Tucson, Arizona MSA
How Does Health Vary Across the Lifespan in the Tucson, Arizona MSA
Lifespan is a fundamental indicator of a community’s overall health and well-being. It reflects not only longevity, but also the conditions that shape one's life: access to care, safe environments, economic opportunity, and social connections. This article, the second in our community health series, examines lifespan as a measure of health across Arizona and the broader MAP region. Understanding the factors that influence longevity can help identify strategies that support longer, healthier lives for all.
Life Expectancy: What the Numbers Reveal
Life expectancy provides a broad measure of overall population health and varies widely across metropolitan areas tracked on the MAP Dashboard. Figure 1 compares life expectancy across the 12 peer MSAs in 2022. San Diego reported the highest life expectancy, at 80.3 years. Austin (78.6), Salt Lake City (78.5), and Denver (77.6) followed closely. Phoenix ranked fifth at 77.5 years, while Tucson placed sixth at 76.5 years. Las Vegas had the lowest life expectancy at 72.1 years, nearly 8 years lower than San Diego. These differences highlight meaningful variation in average lifespan across Tucson’s peer MSAs. The estimates are based on the 2025 County Health Rankings data and represent a three-year average from 2020 to 2022.
Life expectancy measures the average number of years a person is expected to live from birth, based on the age-specific mortality rates observed in a population.
Figure 1: Life Expectancy in Years by MSA (2020-2022)
Understanding Lifespan in Population Health
According to the County Health Rankings & Roadmaps, lifespan is “the period between birth and death” and is a fundamental measure of a community’s overall health. Because it captures the combined effects of social, economic, environmental, and health care factors, lifespan provides insight into differences in health outcomes across populations and highlights where early mortality shortens lives, as deaths in infancy or young adulthood lower average life expectancy.
Economic, social, and environmental factors all play significant roles in shaping lifespan. Social determinants, such as income and education, are closely linked to health outcomes. For example, among adults who survive to age 18, those with at least a master’s degree can expect to live 14.7 more years than those with less than a high school education, and 8.3 more years than those with a high school education¹.
Environmental conditions also influence life expectancy. Exposure to pollution, housing quality, and neighborhood safety can affect the risk of chronic disease, injury, and overall well-being, all of which contribute to differences in longevity across communities.
Premature Mortality by MSA
Several related measures help assess lifespan by capturing both longevity and early mortality. Life expectancy reflects the average number of years people are expected to live. Premature age-adjusted mortality measures the number of deaths among residents under age 75 per 100,000 people, adjusted to account for differences in the age distribution of the population. Child mortality captures deaths among residents under age 20 per 100,000 population, while infant mortality measures deaths within the first year of life per 1,000 live births. Together, these measures allow comparisons across Arizona counties and the 12 western MSAs and help illustrate how early mortality influences overall lifespan.
In 2022, premature age-adjusted mortality varied widely across the 12 MSAs, ranging from 294.0 per 100,000 people in San Diego to 630.6 in Las Vegas. Phoenix fell near the middle of the group, with a rate of 401.0, ranking 5th lowest among the MSAs. Tucson ranked ninth, with a higher rate of 451.3 deaths before age 75 per 100,000 residents.
Figure 2: Premature Age-Adjusted Mortality (Deaths Before Age 75 per 100,000 Residents) by MSA (2022)
Figures 1 and 2 illustrate a clear relationship between premature mortality and life expectancy: areas with higher premature death rates tend to have lower life expectancy. For example, San Diego had the lowest premature mortality and highest life expectancy among the peer western MSAs, while Las Vegas showed the opposite pattern.
Recent national estimates released by the Centers for Disease Control and Prevention (CDC) indicate that U.S. life expectancy increased in the most recent year available. While these national trends provide important context, the analysis presented here focuses on metropolitan comparisons using County Health Rankings data covering the 2020–2022 period.
Child Mortality in Arizona
In 2022, Arizona’s child mortality rate was 56.9 deaths per 100,000 residents under age 20, slightly higher than the U.S. rate of 51.6. Within the state, rates varied considerably across counties. La Paz recorded the highest rate at 112.5, followed by Apache (85.6), Navajo (82.5), and Gila (81.0), all well above both the state and national averages. In contrast, Santa Cruz had the lowest rate at 43.6, below the national rate. Large counties such as Maricopa (54.3) and Pima (56.9) were closer to the statewide average. These differences highlight substantial variation in child mortality outcomes across Arizona.
Figure 3: Child Mortality Rate by Arizona County (2022)
For decades, the United States has reported higher infant mortality rates (IMR) than many other developed nations. In 2021, the U.S. reported 5.4 infant deaths per 1,000 live births, compared with an average of about 4.0 per 1,000 across countries in the Organization for Economic Co-operation and Development (OECD). This placed the United States 33rd out of 38 OECD countries, with only a few OECD countries reporting higher infant mortality rates.
Across Arizona counties, infant mortality rates in 2022 also showed notable variation. The statewide and national averages were 5.6 per 1,000 live births, but several counties exceeded that level. Gila reported the highest rate at 9.2, followed closely by Apache (8.6) and Navajo (8.4). In contrast, Santa Cruz reported the lowest rate at 5.0.
Overall, while Arizona’s average aligns closely with the national rate, disparities across counties highlight areas where targeted public health efforts could help reduce infant mortality and improve early-life health outcomes.
Figure 4: Infant Mortality Rate by Arizona County (2022)
Looking Ahead: The Future of Life Expectancy in the U.S.
While this article focuses on current trends in lifespan across Arizona and the MAP region, it is also important to consider what the future may hold. Recent national forecasts suggest that progress in life expectancy could slow significantly in the coming decades, raising new challenges for public health planning and equity.
A recent analysis from the Institute for Health Metrics and Evaluation (IHME) predicts that U.S. life expectancy gains may stall by 2050, largely due to worsening chronic disease, behavioral risks, and persistent disparities in health outcomes.
According to projections from the Institute for Health Metrics and Evaluation (IHME), Figures 5 and 6 illustrate changes in the leading causes of death in the United States, measured per 100,000 people for both sexes and all ages. Causes of death are grouped into three categories: non-communicable diseases (blue), injuries (green), and communicable, maternal, neonatal, and nutritional diseases (orange).
Figure 5 compares patterns between 1990 and 2025, while Figure 6 shows the projected change from 2025 to 2050. Between 1990 and 2025, non-communicable diseases consistently dominated as the leading cause of death. Respiratory infections and tuberculosis, the only communicable disease in the top seven, remained in seventh place. One notable change during this period is the sharp rise in substance use as a cause of death, moving from 14th place in 1990 to eighth in 2025, while self-harm and violence dropped from eighth to 11th.
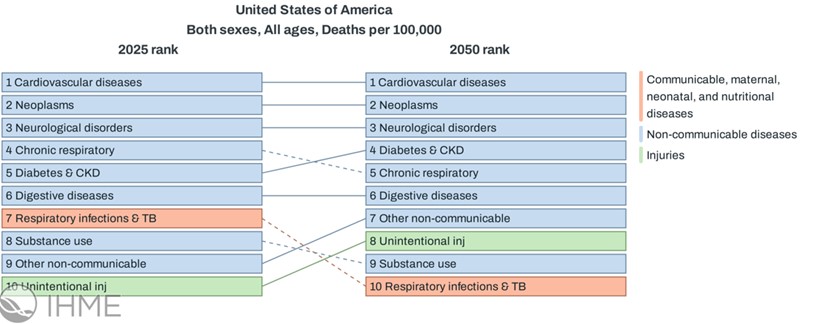
Looking ahead to 2050, projections suggest that non-communicable diseases will continue to dominate the majority of deaths. Diabetes and kidney disease are projected to rise to fourth place, while chronic respiratory diseases decline slightly. Communicable diseases such as respiratory infections and tuberculosis are projected to fall further. Unintentional injuries are expected to rise from 10th to eighth place, while substance use is projected to fall slightly to ninth.
Figure 5: Change in Rank of Leading Causes of Death in the United States: 1990 vs. 2025
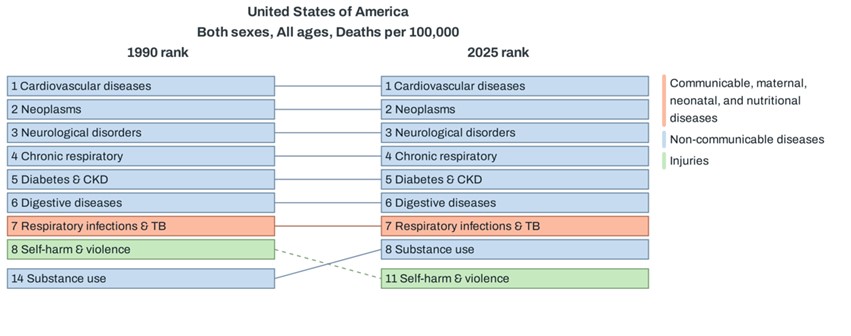
Figure 6: Projected Change in Rank of Leading Causes of Death in the United States: 2025 vs. 2050
Source: Institute for Health Metrics and Evaluation (IHME), Global Burden of Disease Study. Used under Creative Commons Attribution license.
For Arizona, these projections highlight the importance of addressing chronic disease, behavioral risk factors, and persistent health disparities to support continued improvements in life expectancy and long-term population health. Explore the first article in this series, “The Role of Clinical Care in Community Health Infrastructure”.
1Singh GK, Lee H. Marked Disparities in Life Expectancy by Education, Poverty Level, Occupation, and Housing Tenure in the United States, 1997-2014. Int J MCH AIDS. 2021;10(1):7-18. doi: 10.21106/ijma.402. Epub 2020 Dec 30. PMID: 33442488; PMCID: PMC7792745.












